Nanomedicine is the medical application of nanomaterials and nanotechnology. Over the last decade, significant progress has been made in the field of nanomedicines as drug delivery systems for cancer treatment.
The advent of nanomedicines has contributed to the relief of severe side effects of many chemotherapeutics, due to their capability to improve the pharmacokinetics and solubility of those chemotherapies. However, the therapeutic benefits of nanomedicines are moderate in comparison with their parental drugs due to the heterogeneous distributions inside the tumor mass. This is largely caused by the physiological barriers of the solid tumor that hinder the deep penetration of the nanomedicines throughout the tumor.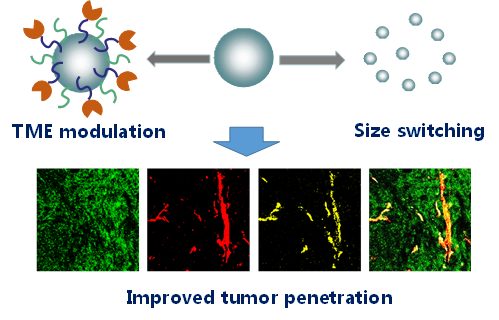
In their review published in WIREs Nanomedicine and Nanobiotechnology, “Strategies to improve tumor penetration of nanomedicines through nanoparticle design,” Ya-Ru Zhang, Run Lin, Hong-Jun Li, Wei-ling He, and Jin-Zhi Du from South China University of Technology and the First Affiliated Hospital of Sun Yat-Sen University highlight the factors that affect the transport of nanoparticles in solid tumors, and elaborate on designing strategies to improve nanoparticle penetration and uniform distribution inside the tumor interstitium.
The authors discuss topics such as abnormal vasculature, elevated interstitial fluid pressure, and dense extracellular matrix (ECM), which intrinsically hinder the transport of nanomedicines in the tumor parenchyma. The review also notes that physiochemical properties of the nanoparticles, such as size, shape, and charge also affect tumor deep penetration.
The endogenous characteristics of the tumor microenvironment such as tumor acidity, overexpression of enzymes, as well as exogenous stimuli such as light, can be utilized to design the stimuli-responsive nanoparticles to overcome delivery obstacles and improve the efficacy of drug delivery. The authors present a series of stimuli-triggered size switching systems, which could shrink their sizes in response to local environment to facilitate tumor transport.
They also discuss a strategy to modulate the tumor microenvironment by conjugating ECM-degrading enzymes on nanoparticles to accelerate tumor penetration of nanomedicines. The deep understanding of tumor biology and the design strategy of nanomedicines is believed to be helpful in future translational studies.
Kindly Contributed by the Authors.