While diseases of the central nervous system (CNS) currently represent a significant health problem, the ongoing rise in the proportion of elderly patients in the population and the current lack of effective treatment strategies will lead to further increases in prevalence in the future.
In the human body, biological “barriers” protect the CNS from external insults, such as drugs and biological agents; however, these same barriers also impede the passage of therapeutic agents that need to reach the CNS to carry out their required activity. Therefore, researchers must discover novel strategies that will permit the delivery of therapies across these barriers to reach the CNS.
Polymer therapeutics, the attachment of an “active agent” to a larger polymer component, represents one promising approach from the field of nanomedicine, with advantages including enhanced blood circulation and enhanced accumulation in the disease area (such as a tumor), fewer off-target side-effects and toxicities, and the possibility of combining two active agents into a single “combination therapy” that may allow for improved patient outcomes and/or disease monitoring.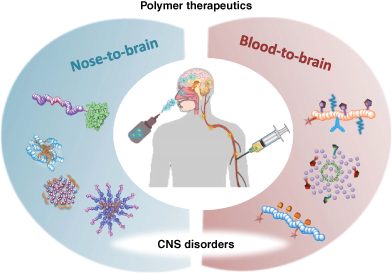
In their review in WIREs Nanomedicine and Nanobiotechnology, Rodriguez-Otormin and colleagues from the Centro de Investigación Príncipe Felipe (CIPF, Valencia, Spain) summarize the most recent and relevant developments, successes, and failures in this field and discuss how we can improve polymer therapeutics-based treatment strategies for various neuro-related disorders and diseases with a focus on non-invasive administration routes such as intranasal and intravenous.
This review pays particular attention to the implications of the biological barriers faced during CNS disease treatment and critically discuss the most frequently applied in vitro/in vivo models for brain delivery screening and how a lack of consensus in data produced from such models currently impedes success in the clinic.
Kindly contributed by the Authors.











